Iron plays a critical role during pregnancy, yet iron deficiency during pregnancy is extremely common. Many women are surprised when routine blood tests show low iron or low hemoglobin, even though they feel they are eating well.
Iron is essential for carrying oxygen in the blood, supporting maternal energy levels, and ensuring proper growth and development of the baby. During pregnancy, the body’s iron needs increase significantly, which is why pregnancy iron levels often drop if intake and absorption are not carefully supported.
What makes iron deficiency challenging is that its symptoms often overlap with normal pregnancy changes. Fatigue, breathlessness, dizziness, or weakness are frequently attributed to pregnancy itself rather than low iron levels. However, when left unaddressed, iron deficiency can progress and affect both the mother and the baby.
This article explains doctor-approved, safe, natural ways to increase iron during pregnancy, focusing on food-first strategies, absorption support, and when medical guidance is essential. Dietary approaches can support treatment, but they do not replace medical advice or prescribed supplementation when needed.
Why Iron Needs Increase During Pregnancy
Increased Blood Volume and Oxygen Demand
During pregnancy, a woman’s blood volume increases by nearly 40–50 percent. This expansion allows more oxygen and nutrients to reach the growing baby. Iron is required to produce haemoglobin, the protein in red blood cells that carries oxygen throughout the body.
As blood volume increases, iron requirements rise to keep hemoglobin levels adequate. Without sufficient iron intake and absorption, hemoglobin levels can gradually fall, leading to iron deficiency during pregnancy.
This increase in iron demand is a normal part of pregnancy. Many women develop low iron, not because they are doing something wrong, but because the body’s needs rise faster than dietary intake and absorption can keep up.
Role of Iron in Fetal Growth and Placenta Development
Iron supports fetal growth by ensuring a steady supply of oxygen through the placenta. Adequate iron levels help the placenta function efficiently, allowing oxygen and nutrients to reach the developing baby throughout pregnancy.
When iron levels are low, oxygen delivery becomes less efficient. This is why doctors closely monitor pregnancy iron levels, especially as the pregnancy progresses, to support healthy fetal growth and development.
Trimester-Wise Iron Requirements
Iron needs change as pregnancy progresses.
In the first trimester, iron demand increases modestly. Some women may show normal hemoglobin levels during early testing due to reduced menstrual blood loss. However, iron stores can still begin to decline quietly during this period.
In the second trimester, iron requirements rise as blood volume expands more rapidly to support both maternal circulation and fetal growth.
In the third trimester, iron needs reach their peak. Rapid fetal growth and increased red blood cell production place the highest demand on iron stores during this time.
Because iron stores can decline gradually, early blood tests may appear normal. This is why iron deficiency is often identified in the second or third trimester rather than at the start of pregnancy.
Signs of Iron Deficiency During Pregnancy
Iron deficiency during pregnancy rarely appears suddenly. In most cases, symptoms develop gradually and may become more noticeable as iron levels continue to fall.
One challenge during pregnancy is that many symptoms of low iron overlap with normal pregnancy changes. Feeling tired, breathless, or low on energy is often assumed to be “just part of being pregnant.” However, when these symptoms persist or become more pronounced, low iron levels may be contributing.
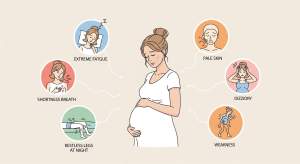
Common low iron pregnancy symptoms include:
• Persistent fatigue that feels more intense than typical pregnancy tiredness
• Pale skin or pale inner eyelids
• Shortness of breath with mild activity
• Dizziness or frequent headaches
• Restless legs, especially at night
• Reduced exercise tolerance or feeling unusually weak
Not every woman will experience all of these symptoms, and some may notice only one or two. This is why symptoms alone are not enough to confirm iron deficiency, and blood tests are important for accurate assessment.
Iron Deficiency vs Anemia During Pregnancy
Iron deficiency and anemia are often used interchangeably, but they are not the same.
Iron deficiency refers to low iron stores in the body. Anemia develops when iron deficiency becomes severe enough to significantly reduce hemoglobin levels, affecting the blood’s ability to carry oxygen.
A woman can have low iron stores without being anemic, especially in the early stages. Blood tests help determine whether iron stores are low, whether anemia is present, or whether both are occurring together. This distinction matters because treatment recommendations depend on the severity of deficiency.
Identifying iron deficiency early allows it to be addressed before it progresses to anemia, making correction simpler and safer during pregnancy.
What Are Normal Iron and Hemoglobin Levels During Pregnancy?
Normal hemoglobin levels during pregnancy vary slightly by trimester and laboratory reference ranges. In general, doctors expect hemoglobin levels to be modestly lower during pregnancy due to increased blood volume, which dilutes red blood cells.
A mild drop in hemoglobin is often a normal physiological change, not a sign that something is wrong. This is why values are always interpreted in the context of pregnancy stage, symptoms, and iron stores rather than a single number.
Some women fall into a “borderline” range where hemoglobin is technically within normal limits, but iron stores are low. These women may still experience symptoms and may be advised to increase dietary iron or begin supplementation under medical guidance.
Because iron requirements change across trimesters, interpreting pregnancy iron levels should always be done with a healthcare provider who can assess trends over time rather than relying on one test result.
Types of Iron: What Pregnant Women Should Know
Heme Iron
Heme iron comes from animal-based foods and is absorbed more efficiently by the body. This means the body can use a higher proportion of the iron consumed.
Common sources include:
• Eggs
• Meat
• Pregnancy-safe fish
Because of its higher absorption, even smaller amounts of heme iron can contribute meaningfully to daily iron needs during pregnancy.
Non-Heme Iron
Non-heme iron comes from plant-based foods. While absorption is lower compared to heme iron, it still plays an important role, especially for vegetarian women, when meals are planned thoughtfully.
Sources include:
• Spinach and leafy greens
• Lentils, chickpeas, rajma
• Dates and raisins
• Nuts and seeds
Non-heme iron is best absorbed when paired with foods that support absorption, which is why meal combinations matter as much as food choices during pregnancy.
Read More: Chia Seed Pudding
Doctor-Approved Natural Ways to Increase Iron
Eat Iron-Rich Foods Daily
Including iron-rich foods for pregnant women consistently is essential. Occasional intake is usually not enough to meet the body’s increasing demands.
Heme iron sources:
• Eggs
• Lean meats
• Fish recommended during pregnancy
Non-heme iron sources:
• Lentils, dals, chickpeas
• Spinach, beetroot
• Dates, figs, raisins
• Nuts and seeds
• Iron-rich Indian vegetables such as drumsticks (moringa)
Read More: Drumsticks (Moringa Pods): Why This Everyday Vegetable Deserves a Spot in Your Diet
For vegetarian women, a well-planned pregnancy diet for iron deficiency can still be effective when iron-rich foods are eaten regularly and absorption is supported.
Improve Iron Absorption Naturally
Iron absorption during pregnancy can be improved with a few simple dietary practices. These small adjustments often make a meaningful difference, even when iron intake remains the same.
Helpful strategies include:
• Pairing iron-rich foods with vitamin C sources like citrus fruits, tomatoes, or amla
• Eating balanced meals rather than isolated foods
• Spreading iron intake across meals instead of concentrating it once daily
In practice, this means focusing on how foods are combined, not just which foods are chosen.
Avoid Iron Absorption Blockers
Certain foods and habits can reduce iron absorption if consumed at the same time.
Common blockers include:
• Tea and coffee
• Large amounts of calcium taken with iron-rich meals
• Certain antacids
This does not mean elimination is necessary. Separating these by one to two hours from iron-rich meals is usually sufficient and more realistic during pregnancy.
Smart Cooking and Eating Practices
Simple everyday habits can quietly support iron intake:
• Avoid overcooking leafy greens, which can reduce nutrient content
• Eat freshly prepared meals when possible
• Maintain regular meal timing
Some households also use iron cookware, which may modestly increase iron content in food. While helpful, this should be seen as a supporting habit rather than a primary strategy.
Indian Diet Plan Tips for Pregnancy Iron Support
An Indian pregnancy diet for iron deficiency can be both effective and culturally familiar.
Examples include:
• Dal with lemon and vegetables
• Vegetable sabzi paired with vitamin C-rich chutney
• Whole grains combined with lentils and vegetables
• Dates or raisins as small snacks
Portion sizes should remain moderate, and adjustments may be needed as pregnancy progresses.
Can You Increase Iron Without Supplements?
Many women ask whether it is possible to rely only on food.
Food-first approaches may be sufficient for mild deficiency or maintenance. However, supplements are often recommended when:
• Iron deficiency is moderate or severe
• Hemoglobin levels are low
• Absorption is impaired
Doctors prescribe supplements because pregnancy increases iron needs beyond what diet alone can sometimes provide. These are safe ways to increase iron in pregnancy when taken as directed.
Common Myths About Iron During Pregnancy
There is a lot of confusion around iron intake during pregnancy, which can create unnecessary fear or hesitation. Clarifying these common myths helps women make informed decisions with confidence.
- Iron-rich foods cause excessive weight gain – False. Iron-rich foods support oxygen delivery and energy levels. Weight gain during pregnancy is influenced by overall nutrition, not iron intake alone.
- Plant foods do not help iron levels – False. While plant-based iron is absorbed less efficiently, it still contributes meaningfully when meals are planned well and paired with absorption-supporting foods.
- Iron always causes constipation – Not always. Food-based iron is less likely to cause constipation, and even supplements can often be adjusted to improve tolerance.
- Iron supplements harm the baby – False when medically prescribed. Supplements are commonly recommended during pregnancy and are considered safe when taken under medical guidance.
Understanding these myths helps reduce unnecessary worry and supports healthier choices during pregnancy.
When to Consult a Doctor
While mild iron deficiency can often be supported with diet and lifestyle changes, there are situations where medical evaluation is important.
Consult a doctor if there is:
• Very low hemoglobin levels
• Breathlessness at rest or with minimal activity
• Palpitations or persistent dizziness
• Concerns about fetal growth
• No improvement in iron levels despite dietary changes
These situations require medical assessment and should not be managed with food alone.
Conclusion
Iron needs increase naturally during pregnancy, and iron deficiency during pregnancy is common. A food-first, doctor-approved approach that focuses on iron-rich foods, improved absorption, and consistent eating habits can help support healthy pregnancy iron levels.
At the same time, diet complements medical care and does not replace it. With timely testing, guidance, and appropriate treatment when needed, iron deficiency is manageable and rarely permanent. Supporting iron levels helps protect maternal energy, fetal growth, and overall pregnancy health throughout pregnancy.
Understanding how your body responds to food, absorption, and changing nutrient needs during pregnancy helps turn nutrition into a system rather than guesswork. Platforms like Alpha Coach help people access reliable nutrition information and make informed food choices, supporting consistency and confidence throughout different life stages, including pregnancy.













Leave a Reply